MedComm | Low hemoglobin is associated with worse outcomes via larger hematoma volume in intracerebral hemorrhage due to systemic disease

Open the phone and scan
Whether hemoglobin is associated with outcomes of a specific subtype of intracerebral hemorrhage (ICH) is unknown. A total of 4643 patients with ICH from a multicenter cohort were included in the analysis (64.0% male; mean age [SD], 58.3 [15.2] year), of whom 1319 (28.4%) had anemia on admission. The unsupervised consensus cluster method was employed to classify the patients into three clusters. The patients of cluster 3 were characterized by a high frequency of anemia (85.3%) and mainly composed of patients of systemic disease ICH subtype (SD-ICH; 90.0%) according to the SMASH-U etiologies. In SD-ICH, a strong interaction effect was observed between anemia and 3-month death (adjusted odds ratio [aOR] 4.33, 95% confidence interval [CI] 1.60–11.9, p = 0.004), and the hemoglobin levels were linearly associated with 3-month death (aOR 0.75, 95% CI 0.60–0.92; p = 0.009), which was partially mediated by larger baseline hematoma volume (p = 0.008). This study demonstrated a strong linear association between low hemoglobin levels and worse outcomes in SD-ICH, suggesting that hemoglobin-elevating therapy might be extensively needed in a specific subtype of ICH.
The variance may relate to the heterogeneity of the ICH patients of different natural histories and associated risk factors, but there is little knowledge of which factors could define the subgroup with a specific demand for hemoglobin. Authors hypothesized that different ICH subgroup patients have specific demands for hemoglobin. Here, in a large prospective multicenter cohort study of patients with ICH, they investigated whether ICH patients have different demands of hemoglobin using the unsupervised consensus cluster method and further explore its clinical significance.
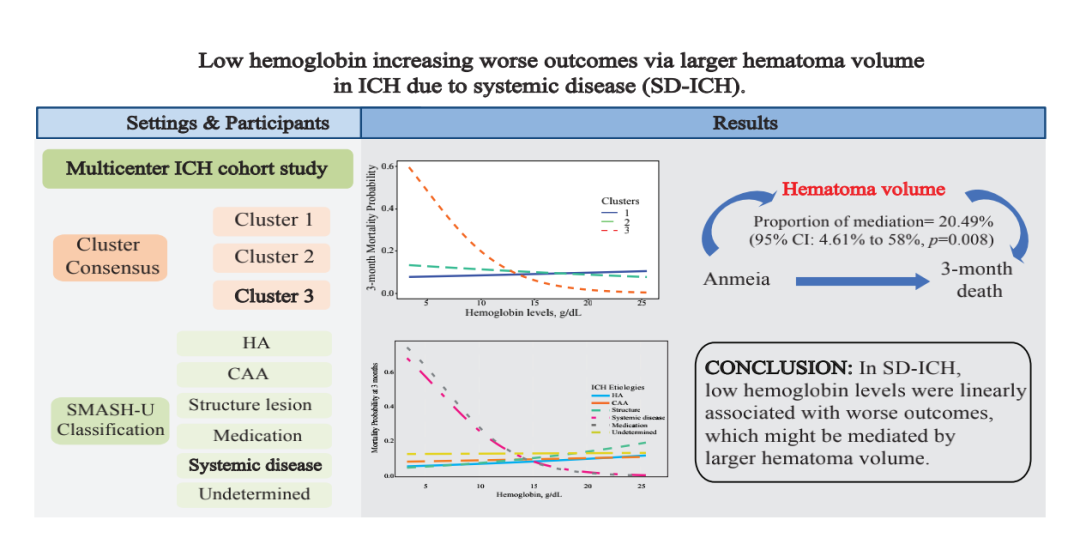
Research methods and main results
Article Access: https://doi.org/10.1002/mco2.96
Website for MedComm: https://onlinelibrary.wiley.com/journal/26882663
Looking forward to your contributions.


